Audit of disease modifying treatments of multiple sclerosis at Royal Preston Hospital

Royal Preston Hospital is the regional centre for neurology in Lancashire, with a population over one million. The treatment of multiple sclerosis is centralised here, and all disease modifying treatments are prescribed and monitored from within the service. There has been no previous database kept of this large cohort of patients. The creation of accurate records will allow us to continually audit this specialised and costly management, and enable us to achieve greater efficiency, and clinical care. Our aim was to create a database of patients with multiple sclerosis on disease modifying treatments (DMTs). We present the initial results from this database, which continues to grow in size. By presenting this data, we aimed to identify what DMTs were used and under what circumstances. This will allow us to compare our activity to national standards, and other MS centres.
Methods
A sample of 253 patients was collected at random from the cohort of DMT patients. We used clinic letters to obtain our information. We recorded gender; age; first- and second-line disease modifying treatments chosen; the number of relapses experienced on each treatment; and most up to date Expanded Disability Status Scale (EDSS).
Results
192 patients were female, and 57 were male. 90 patients had two relapses before commencing a DMT, followed by 40 patients with three relapses, 23 with one relapse, seven with four relapses, and four with five relapses. 89 patients did not have sufficient information regarding relapses in clinical records.
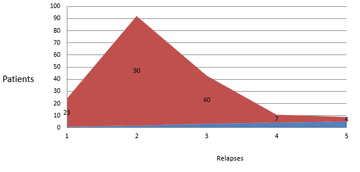
Number of relapses before commencing a DMT
The first-line disease modifying treatments that were used, in order of frequency, were copaxone [62], avonex [48], betaferon [39], rebif [39], tecfidera [25], tysabri [11], plegridy [6], mitoxanthrone [6], extavia [4], fingolimod [1], teriflunomide [1].
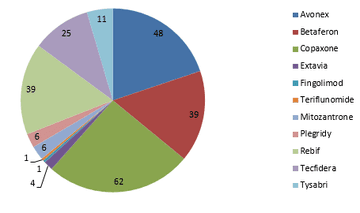
First-line DMTs
One hundred and two patients had no relapse on first choice DMT. Two patients developed into secondary progressive multiple sclerosis.
The number of relapses before escalation to another DMT were: 42 patients with a single relapse; 29 patients with two relapses; 13 patients with three relapses; six patients with four relapses; four patients with five relapses; and one patient with six relapses. Forty-five patients had insufficient clinical records to identify this.
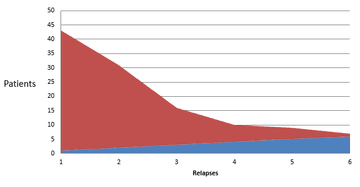
Number of relapses before escalation of DMT
Conclusions
Within our cohort of patients on a disease modifying treatment for MS, the majority were female. Most commonly two relapses were seen prior to commencing a first-line disease modifying treatment. Copaxone was the most widely used disease modifying treatment. Patients escalated DMT most commonly after a single relapse. Difficulties in establishing a clear timeline for patients using the medical records restricts our knowledge, however broadly the findings are in keeping with guidelines regarding escalation.
Recommendations
We will continue to collect data from this large cohort. Therefore we will repeat this audit with a larger population size. We will repeat these observations, in addition assessing most recent EDSS, and consultant choice of disease modifying treatment. Following this we will present the findings to staff, and discuss the implications of cost, and perceived impact of quality of patient care.
More MS Academy Medication Projects
Encouraging excellence, developing leaders, inspiring change
MS Academy was established five years ago and in that time has accomplished a huge amount. The six different levels of specialist MS training are dedicated to case-based learning and practical application of cutting edge research. Home to national programme Raising the Bar and the fantastic workstream content it is producing, this is an exciting Academy to belong to.

